Reviewed by Sahil Chopra, MD, and Stacey Gunn, MD.
Research by Savit Malhotra.
Introduction
Over the last two months, we have spent some time discussing the many different relationships that sleep apnea shares with the body. This week, we conclude our series on these relationships by talking about bruxism. However, we also want to share that the list of relationships extends far beyond what we have talked about. The issue is that many of these relationships lack extensive and definitive evidence. So while we may know that these relationships exist, we may lack understanding of why they do or what the pathophysiology is. As more evidence becomes available, we will continue to share these findings with you to keep you all well informed.
What can be said though is that the best course of action when it comes to sleep apnea is to treat the disease. While we may not know everything about the effects of sleep apnea, we do know there are negative consequences to leaving it untreated. For this reason, we always recommend that, if you have sleep apnea, you see a medical provider to discuss a treatment plan that works best for you.
What is Bruxism?
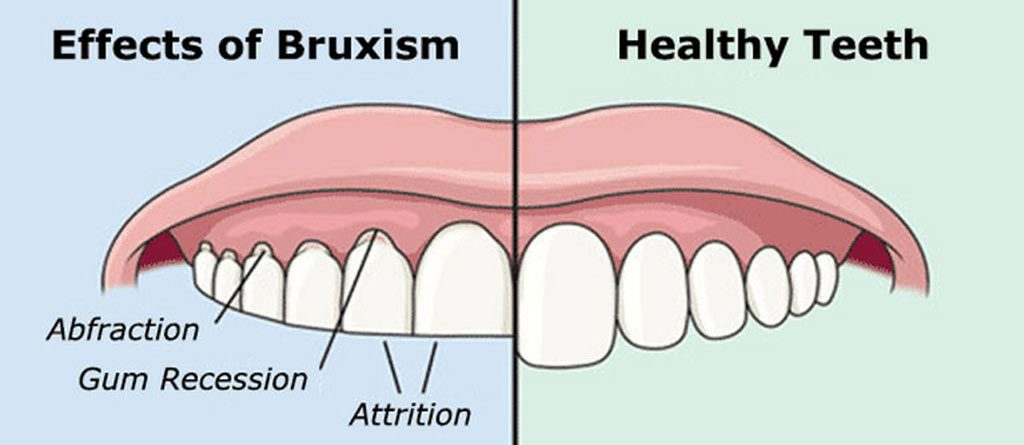
Bruxism is a condition where you, subconsciously, grind your teeth, causing damage to your teeth. Bruxism can happen both while you’re awake and during sleep, and due to its prevalence of occurring during sleep, it is hard to say how many people actually have bruxism, and many people are unaware that they have it until their dentist lets them know.[1] This teeth grinding can lead to the enamel of the teeth (the outermost layer) becoming worn and the inner layers being exposed. The tooth may become flattened or chipped, leading to pain or sensitivity. Additionally, a person’s jaw may also become sore, and the muscles may tighten. Also common effects of bruxism are headaches, earaches, and problems sleeping.[2]
Typically, children are more likely to develop bruxism than adults, with studies showing variability in the rates, ranging from 5.9% to 49.6% of children aged 0 to 17 years old have some degree of bruxism. Males appear to have a slightly higher risk of developing bruxism compared to females (18.9% of males compared to 16.2% of females).[3] Common risk factors of bruxism include stress, anxiety, family history of the disease, other chronic biting habits, and emotional distress.[4] Aside from sleep apnea, there are also a number of other medical conditions that can cause bruxism, including dementia, ADHD, night terrors, Parkinson’s disease, gastroesophageal reflux disorder, and epilepsy.[4]
How Do the Two Worsen Each Other?
It has been found that 33% to 54% of those with sleep apnea have bruxism, indicating that there is a strong correlation between the two diseases.[5] However, what is still not entirely clear is the pathophysiology between the two diseases. There are several theories behind the relationship, but no definitive answer has been reached. One leading theory behind the correlation relates to the body trying to find ways to breathe while the airway is blocked. Those with sleep apnea will experience either a partial or complete blockage of their airway. However, the human body is resilient, and it will try to compensate for this blockage by moving the tongue around by either grinding the teeth or clenching the jaw. In doing so, the airway is able to open again, and a person is able to once again breathe normally.[7] Another key theory is that those with sleep apnea often experience micro-arousals during sleep, leading to their nervous system (specifically their autonomic nervous system) being triggered. As we have discussed, the autonomic nervous system is responsible for the fight-or-flight response, and part of this response during sleep involves jaw movement and teeth grinding.[5] Interestingly, this theory is also somewhat related to the idea of oxidative stress. For more information about what oxidative stress is, we encourage you to read some of our other articles, such as the relationship between sleep apnea and stroke.
We have spent a long time talking about bidirectional relationships, but this may not be the case here. Teeth grinding likely does not cause sleep apnea because it doesn’t make sense for this disease to obstruct the airway in any way. However, we will note that recent studies have found a correlation between bruxism and oxidative stress. These studies showed that those with sleep bruxism had higher levels of key markers of oxidative stress (not to say there is causation, but instead correlation).[6] In past articles, we have mentioned that oxidative stress could be an explanation behind why certain diseases cause sleep apnea, but even this theory has not been fully proven. Based on the current literature, it is a slight overstatement to say that bruxism causes sleep apnea.
What Should I Look Out For?
As we discussed in the previous article, the STOPBANG method remains an effective way for a person to help screen themself to see if they have sleep apnea. This test/acronym (posted below for reference) isn’t perfect, but it is still an incredibly useful tool.
- S - Snoring
- T - Tiredness during the day
- O - Obstruction (brief pause in breathing while sleeping)
- P - Pressure (high blood pressure)
- B - Body mass index of 30 or greater
- A - Age of 50+
- N - Neck circumference of greater than 16 inches (in women) or 17 inches (in men)
- G - Gender (male)
If you have three or more of the above-mentioned characteristics of sleep apnea, it is important that you see a sleep medicine doctor so that they can properly diagnose you and you can begin treatment. However, we will also mention that it is possible to have sleep apnea even with a low STOPBANG score, and so a normal score should not prevent someone from being evaluated if they are otherwise concerned.[8]
Those with bruxism may experience jaw, neck, or face pain/soreness. They may also notice that their jaw muscles may begin to enlarge, and they may experience pain that feels like it is in the ear or a dull headache starting at the temples. Furthermore, those with bruxism may notice their teeth look flattened or they have a new pain or sensitivity in their teeth. Lastly, a bed partner may hear a grinding noise while they are sleeping that could be indicative of bruxism. Any of these symptoms is worth noting and mentioning to a professional, such as a dentist.[2]
What can I do about my Bruxism?
Typically, a dentist or oral surgeon would be the best person to ask if you are worried about having bruxism. They can examine your tooth enamel and determine if it has been ground away or if you have any damage to the teeth that could be due to teeth grinding. If your doctor has determined you do have bruxism, then they may recommend a splint or mouth guard, physical barriers that will prevent your teeth from grinding against each other. However, sometimes the solution is a lifestyle change. For example, if you are experiencing a period of high stress, seeking therapy to help you manage that stress can help resolve your bruxism. Medications do exist as well, such as muscle relaxants and Botox injections, to help limit the movement of the jaw and thus prevent bruxism.[2]
As we have discussed, the cause of your bruxism can also be sleep apnea. If you have sleep apnea, it is best that you resolve that apnea to help mitigate or even prevent yourself from developing bruxism. Unfortunately, damage done to the teeth is permanent.[9] For this reason, we recommend not waiting since doing so can lead to further damage. Your teeth are precious, and it is best to protect them in any way that you can, and part of that treatment is resolving your sleep apnea.

Conclusion
Sleep apnea is a complex disorder, and there is much we still don’t know and much we may never know. However, what we do know is that sleep apnea is serious. The data shows that those with sleep apnea are at a significantly higher risk of developing some other disease. We hope that, over the past two months, we have made you well informed of the different conditions that share a relationship with sleep apnea. If you are worried you may have sleep apnea, or already know that you do, it is best to see a doctor so that they can help you come up with a plan to improve your sleep and reduce your apnea. By doing so, you may be able to significantly decrease your risk of developing some other adverse condition. The Empower Sleep team is always available to help you with any questions you may have. If you are curious to learn more, please see our about page to begin scheduling with one of our sleep experts!