Chronic sleep deprivation is a pervasive issue that occurs when an individual consistently fails to get the recommended amount of sleep, typically 7-9 hours for adults. This insufficient sleep can be due to a variety of factors, such as lifestyle choices, work demands, or sleep disorders. Over time, chronic sleep deprivation can lead to a myriad of health problems, both physical and mental.
Let’s delve into the long-term effects of chronic sleep deprivation on an individual's health and provide practical, science-backed strategies for reducing these detrimental consequences. By addressing the issue of sleep deprivation, readers can better understand the importance of prioritizing sleep and make informed choices to improve their overall well-being.
Physical health effects:
- Obesity and weight gain: Research has shown that people who consistently experience sleep deprivation are at a higher risk of obesity and weight gain. This is primarily because lack of sleep can disrupt the balance of hormones responsible for regulating appetite, such as leptin and ghrelin, resulting in increased hunger and food consumption.
- Diabetes and insulin resistance: Chronic sleep deprivation can also lead to an increased risk of type 2 diabetes. A study published in The Lancet found that people who slept less than six hours per night were at a higher risk of developing impaired glucose tolerance, a precursor to diabetes. This occurs because sleep deprivation affects the body's ability to metabolize glucose, leading to insulin resistance.
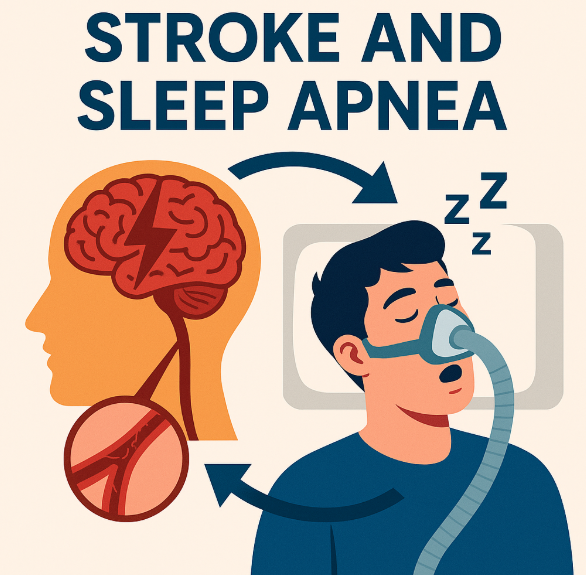
- Cardiovascular diseases: Insufficient sleep has been associated with an increased risk of various cardiovascular diseases, including hypertension, coronary heart disease, and stroke. This is due to the fact that sleep deprivation can cause inflammation, elevated blood pressure, and an increase in stress hormones, all of which contribute to the development of heart-related issues.
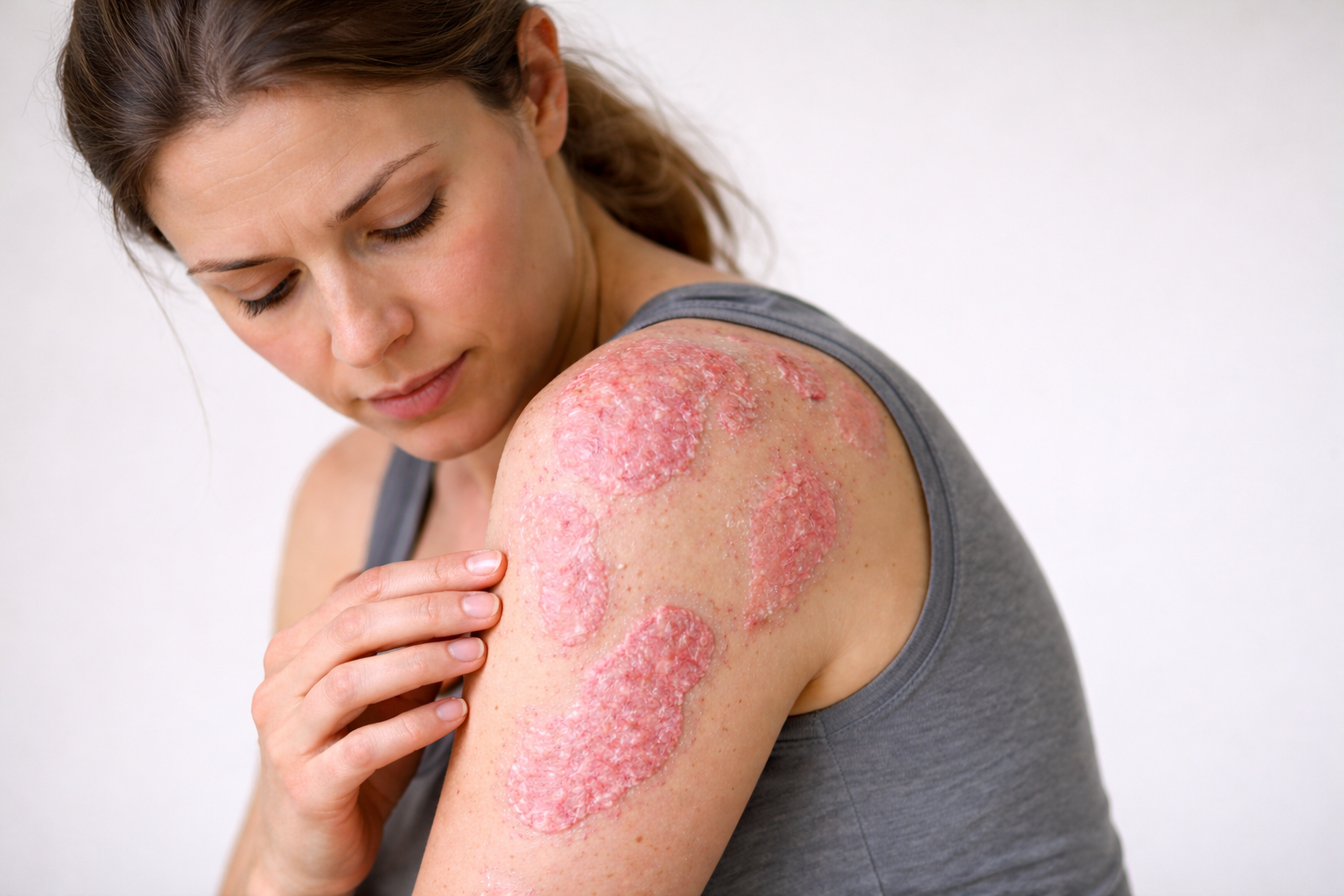
- Weakened immune system: Sleep is essential for maintaining a strong immune system, as it aids in the production of infection-fighting cells and cytokines. Prolonged sleep deprivation can weaken the immune system, making individuals more susceptible to infections and illnesses.
- Hormonal imbalances: Chronic sleep deprivation can lead to hormonal imbalances, such as those affecting the production of cortisol, growth hormone, and melatonin. These imbalances can have various negative effects on the body, including increased stress, impaired tissue repair, and disrupted circadian rhythms.
Mental health effects
- Anxiety and depression: There is a strong link between sleep deprivation and increased risk of anxiety and depression. Research shows that individuals who experienced insomnia were more likely to develop depression and anxiety disorders.
- Cognitive decline and memory issues: Sleep plays a crucial role in memory consolidation and cognitive function. Chronic sleep deprivation can lead to difficulties in learning, concentration, and memory retention. People who suffer from long-term sleep deprivation are more likely to experience cognitive decline and memory impairment.
- Increased risk of Alzheimer's disease: Studies have suggested that chronic sleep deprivation may contribute to the development of Alzheimer's disease. This is because sleep is necessary for the clearance of beta-amyloid, a protein that accumulates in the brains of Alzheimer's patients. Insufficient sleep can lead to an increased buildup of this protein, potentially increasing the risk of developing the disease.
- Impact on emotional regulation and mood: Sleep deprivation has been found to negatively affect emotional regulation and mood. A study found that individuals who were sleep deprived had heightened emotional reactivity to negative stimuli, making it more difficult for them to effectively manage their emotions. This can lead to increased irritability, mood swings, and a decreased ability to cope with stress.
.png)
Tips for Reducing Chronic Sleep Deprivation
One of the most effective ways to combat chronic sleep deprivation is to establish a consistent sleep schedule. Going to bed and waking up at the same time every day, even on weekends, helps regulate the body's internal clock and makes it easier to fall asleep and wake up feeling refreshed. Consistency in sleep patterns has been shown to improve sleep quality and overall sleep duration.
Create a conducive sleep environment
- Cool, dark, and quiet: Ensuring that the sleep environment is cool, dark, and quiet can significantly improve sleep quality. Research suggests that a cooler room temperature (around 60-67°F or 16-19°C) is optimal for sleep, as it facilitates the body's natural cooling process during sleep. Using blackout curtains and minimizing noise can also help create a more conducive sleep environment.
- Comfortable bedding: Investing in comfortable bedding, including a supportive mattress and pillows, can make a significant difference in sleep quality. Research has shown that individuals who sleep on a comfortable mattress report better sleep quality and reduced back pain.
- Limiting electronics before bedtime: Exposure to the blue light emitted by electronic devices, such as smartphones and tablets, before bedtime can disrupt the production of melatonin and make it more difficult to fall asleep. Limiting the use of these devices at least an hour before bedtime can help improve sleep quality.
Prioritize relaxation techniques
- Meditation and mindfulness practices: Incorporating meditation and mindfulness practices into one's daily routine can help promote relaxation and improve sleep quality. Studies found that mindfulness-based stress reduction techniques, such as meditation, improved sleep quality in adults with sleep disturbances.
- Deep breathing exercises: Deep breathing exercises, such as diaphragmatic breathing and the 4-7-8 breathing technique, can help calm the nervous system and facilitate sleep.
- Progressive muscle relaxation: Progressive muscle relaxation is a technique that involves tensing and relaxing various muscle groups in the body to promote relaxation and reduce stress. Research has shown that this technique can be effective in improving sleep quality.
Adopt healthy sleep habits
- Limit caffeine and alcohol intake: Consuming excessive amounts of caffeine and alcohol can negatively affect sleep quality. Caffeine is a stimulant that can make it difficult to fall asleep and stay asleep, while alcohol can disrupt the sleep cycle and impair restorative sleep. Limiting the intake of these substances, particularly in the hours leading up to bedtime, can improve sleep quality.
- Engage in regular physical activity: Regular physical activity has been shown to improve sleep quality and increase sleep duration. Engaging in moderate-intensity exercise, such as walking, swimming, or yoga, for at least 150 minutes per week can help promote better sleep.
- Avoid Eating heavy meals close to bedtime can cause discomfort and make it difficult to fall asleep. It is recommended to finish eating at least two hours before bedtime to allow the body ample time to digest the food.
Seeking Professional Help
.png)
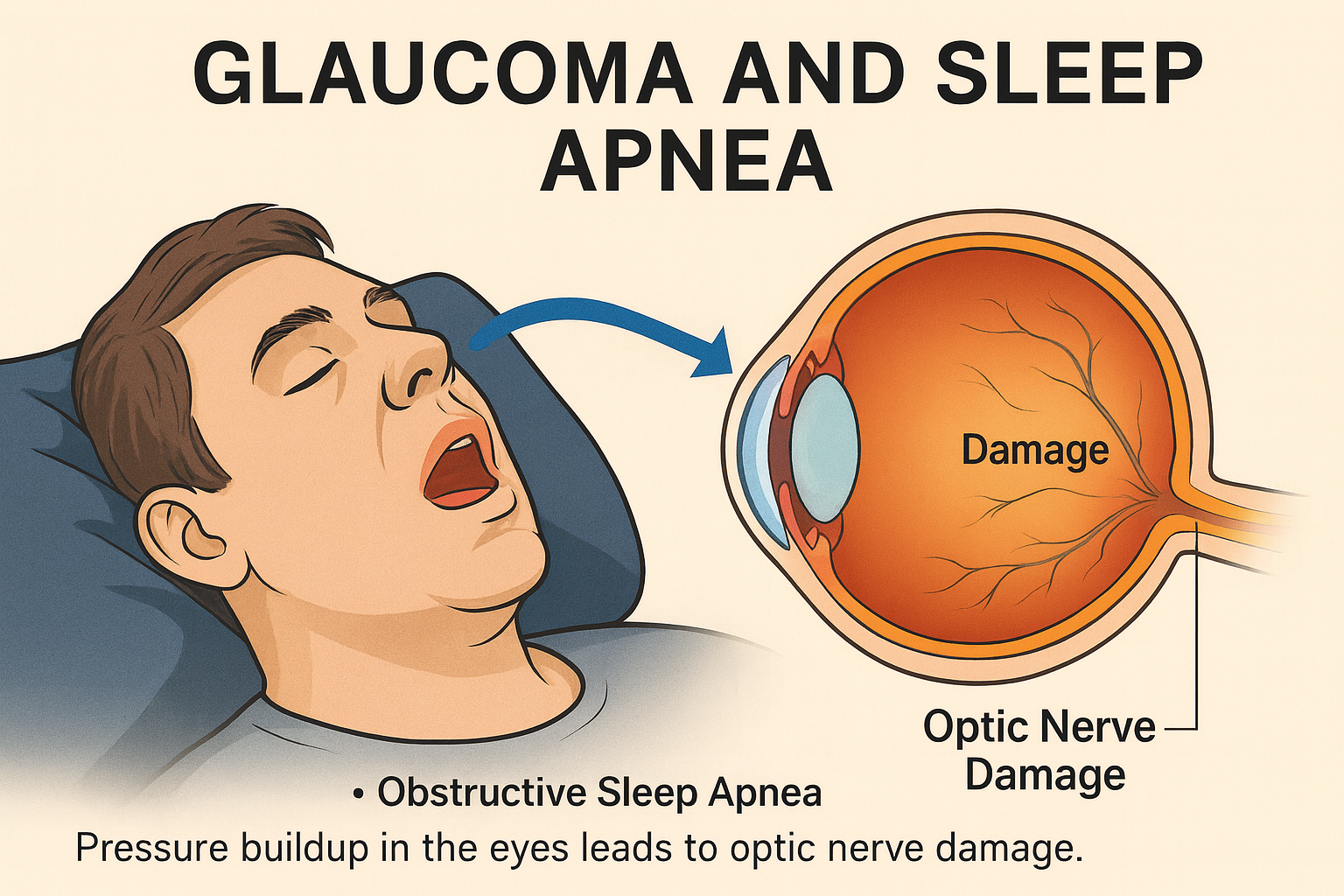
Despite implementing various strategies to improve sleep quality, some individuals may continue to experience chronic sleep deprivation. In such cases, it is important to consult a sleep specialist to determine if an underlying sleep disorder, such as insomnia, sleep apnea, or restless legs syndrome, is responsible for the ongoing sleep issues. Warning signs that may indicate a need for professional help include consistently struggling to fall asleep or stay asleep, excessive daytime sleepiness, loud snoring, or difficulty breathing during sleep.
Depending on the specific sleep disorder diagnosed, a sleep specialist may recommend one or more of the following treatment options:
- Cognitive-behavioral therapy for insomnia (CBT-I): CBT-I is an evidence-based treatment for insomnia that focuses on identifying and modifying negative thoughts and behaviors that contribute to sleep problems. This therapy has been shown to be effective in improving sleep quality, reducing sleep latency, and decreasing the frequency of nighttime awakenings.
- Sleep medications: In some cases, sleep specialists may prescribe medications to help individuals fall asleep or stay asleep. These medications can include benzodiazepines, non-benzodiazepine hypnotics, and melatonin receptor agonists. While these medications can be effective in the short term, they may also have potential side effects and can be habit-forming. It is important to use sleep medications under the supervision of a healthcare professional and to explore other treatment options when appropriate.
- Lifestyle modifications: In addition to the tips mentioned earlier in this blog, a sleep specialist may recommend further lifestyle modifications to address specific sleep disorders. For example, individuals with sleep apnea may be advised to lose weight or use a continuous positive airway pressure (CPAP) machine to improve their breathing during sleep. Similarly, individuals with restless legs syndrome may be advised to avoid caffeine and alcohol, engage in regular exercise, and maintain a consistent sleep schedule.
Conclusion
Addressing chronic sleep deprivation is of paramount importance for maintaining overall health and well-being. As we have discussed, insufficient sleep can lead to a multitude of physical and mental health issues, including obesity, diabetes, cardiovascular diseases, cognitive decline, and mood disorders. By understanding the science behind sleep deprivation and its long-term effects on health, individuals can make informed decisions and take appropriate steps to prioritize their sleep.
We encourage readers to prioritize sleep for better long-term health by implementing the practical tips and strategies outlined in this blog. If you continue to struggle with sleep issues despite making these changes, don't hesitate to seek professional help from a sleep specialist, such as those at Empower Sleep. Our mission is to make sleep care accessible and affordable, offering convenient at-home sleep testing, virtual consultations, and personalized treatment options to help you achieve better sleep and lead a healthier life. To learn more about our services and how we can support your journey to better sleep, visit empowersleep.com. Together, let's transform your sleep and empower your life.
References
- Baglioni, C., Battagliese, G., Feige, B., Spiegelhalder, K., Nissen, C., Voderholzer, U., Lombardo, C., Riemann, D. (2011). Insomnia as a predictor of depression: a meta-analytic evaluation of longitudinal epidemiological studies. Journal of Affective Disorders, 135(1-3), 10-19. https://doi.org/10.1016/j.jad.2011.01.011
- Besedovsky, L., Lange, T., Haack, M. (2012). The sleep-immune crosstalk in health and disease. Physiological Reviews, 92(3), 1089-1125.
https://pubmed.ncbi.nlm.nih.gov/30920354/ - Black, D. S., O'Reilly, G. A., Olmstead, R., Breen, E. C., & Irwin, M. R. (2015). Mindfulness meditation and improvement in sleep quality and daytime impairment among older adults with sleep disturbances: a randomized clinical trial. JAMA Internal Medicine, 175(4), 494-501. https://doi.org/10.1001/jamainternmed.2014.8081
- Cajochen, C., Frey, S., Anders, D., Späti, J., Bues, M., Pross, A., Mager, R., Wirz-Justice, A., Stefani, O. (2011). Evening exposure to a light-emitting diodes (LED)-backlit computer screen affects circadian physiology and cognitive performance. Journal of Applied Physiology, 110(5), 1432-1438. https://doi.org/10.1152/japplphysiol.00165.2011
- Cappuccio, F. P., Cooper, D., D'Elia, L., Strazzullo, P., & Miller, M. A. (2011). Sleep duration predicts cardiovascular outcomes: a systematic review and meta-analysis of prospective studies. European Heart Journal, 32(12), 1484-1492. https://doi.org/10.1093/eurheartj/ehr007
- Ditto, B., Eclache, M., & Goldman, N. (2006). Short-term autonomic and cardiovascular effects of mindfulness body scan meditation. Annals of Behavioral Medicine, 32(3), 227-234. https://doi.org/10.1207/s15324796abm3203_9
- Gottlieb, D. J., Punjabi, N. M., Newman, A. B., Resnick, H. E., Redline, S., Baldwin, C. M., Nieto, F. J. (2005). Association of sleep time with diabetes mellitus and impaired glucose tolerance. Archives of Internal Medicine, 165(8), 863-867. https://doi.org/10.1001/archinte.165.8.863
- Gujar, N., McDonald, S. A., Nishida, M., & Walker, M. P. (2011). A role for REM sleep in recalibrating the sensitivity of the human brain to specific emotions. Cerebral Cortex, 21(1), 115-123 https://doi.org/10.1093/cercor/bhq064
.png)